As a provider using a clearinghouse or vendor for Medicare eligibility verification, you have a firm deadline looming. On May 11, 2026, CMS plans to roll out a new HETS trading partner management system, and all providers must be enrolled in the system by submitting a HETS EDI enrollment attestation prior to that date.
The enrollment connects each one of your National Provider Identifier(s) (NPIs) to the vendors performing the eligibility queries for your patients. Any eligibility requests made after May 11, 2026, from a vendor performing an eligibility query on your behalf that are linked to your NPI(s) will be rejected without any exception. For billing teams responsible for the front-end revenue cycle functions, this is not a back-office IT function - this is a patient access and cash flow emergency.
What Is the HETS EDI Attestation Deadline?
- CMS has mandated that all providers must attest their NPI via HETS EDI by May 11, 2026.
- The purpose of completing a HETS EDI attestation is to link each provider's NPI with the clearinghouse or vendor through which the Medicare 270/271 eligibility transaction is performed.
- If an NPI remains unattested, it will be rejected from performing Medicare eligibility inquiries with an AAA Error Code of "41" - Hard Stop - No Exceptions.
- All multi-location practices are required to complete attestation on each NPI as there is no option to perform attestation in bulk or group-level option.
What Is the HETS System, and Why Does This Matter?
HETS stands for the 'HIPAA Eligibility Transaction System'. Providers and suppliers are required to register into the HETS Electronic Data Interchange (EDI) to verify Medicare beneficiary eligibility. In most cases, most practices do not interact with HETS; their clearinghouses, billing software, or eligibility vendors do this for them by using 270 Inquiry and 271 response transactions.
This working relationship has operated silently over the years. This new policy adds an additional level of accountability. The CMS has now required all provider organizations to formally verify that any clearinghouse or third-party checking Medicare eligibility for them has the approval to do so. The goal here is transparency: CMS via your Medicare Administrative Contractor (MAC) wants a documented, verifiable record of which entities are using your beneficiaries information on your behalf.
Here's how this affects you in real terms. As an example, even though your clearinghouse may have checked Medicare eligibility for your office over the last several years, without formal documentation as related to each of your NPIs, that will be stopped by CMS on May 11.
What Changed, and When Does Enforcement Begin?
Beginning on May 11, 2026, CMS will switch to a new HETS (Healthcare Electronic Transaction System) trading partner management system. After that date, any NPI without an active enrollment will have its eligibility requests rejected outright. There is no grace period.
The enforcement mechanism for this issue is AAA Error Code "41". This error code means there is no established or validated relationship between the NPI and their third-party vendors, which could possibly be caused by incomplete enrollment.
As of March 31, 2026, CMS now requires provider organizations to confirm that any clearinghouse or third-party checking Medicare eligibility for them is approved to do so. The window is closing fast. If your team hasn't acted yet, the time is now.
Another piece of information you should know regarding the completion of attestation is that for each billing NPI an organization enrolls with CMS for purposes of Medicare eligibility checks; there is no mass (bulk) attestation across multiple NPIs. In addition, the clearinghouse CANNOT complete this action on behalf of the provider.
What This Means for Your Revenue Cycle
Let's break down the downstream damage if attestation gets missed.
Medicare eligibility verification (the initial step in the Healthcare Revenue Cycle Management Services), When fails, nothing upstream can fix it; therefore, you will have no knowledge of the patient's coverage status, their deductible or how they are going to pay for the care received prior to arrival. The result is incorrect patient liability estimates at the point of registration/check-in, increased denials after submission of claims due to lack of verified information, and ultimately an administrative burden on the staff to perform individual eligibility verifications manually using the MAC portal.
A disruption in Medicare eligibility inquiries creates immediate secondary consequences for claims processing; i.e., claim denials increase, patient liability estimations become unreliable, and staff is required to perform individual work-arounds to continue the entire front-end process.
A larger health system with many facilities and NPIs has more potential for errors because each site is required to have attestation completed in order to provide attestations for all NPI's. In addition, since it may take more planning to coordinate this effort among locations (and possibly even more lead time), larger health systems should begin now - not wait until next week - if their billing is done using many individual or group NPI's.
A denial management services team can clean up the mess after the fact, but no amount of appeals work can offset a total freeze on eligibility verification across your Medicare patient population.
What Should Your Practice Do Before May 11?
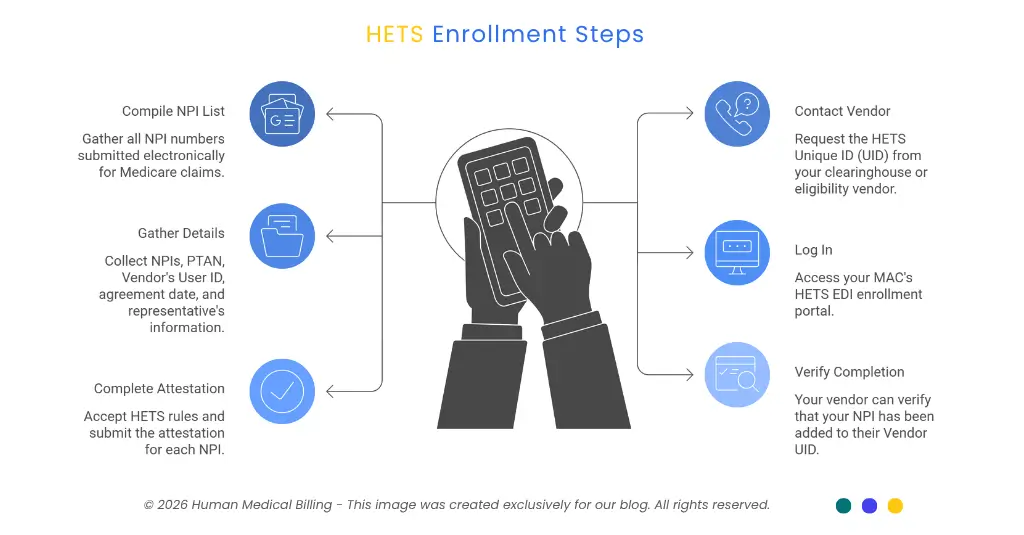
The main point is that it can take anywhere from 5-15 minutes to complete the attestation for each NPI number once you have all the correct information in place. It's really the preparation part that will be a time commitment, especially with larger organizations.
1. Compile your full NPI list.
All NPI numbers that are submitted electronically for claims to Medicare MUST have an identical NPI number in the HETS enrollment process.
2. Contact your clearinghouse or eligibility vendor.
Request their HETS Unique ID (UID). All providers need to identify which vendors do Medicare eligibility checks on their behalf and initiate the attestation process as early as possible.
3. Gather required enrollment details.
In addition, you will also need to provide your NPIs, your Provider Transaction Access Number (PTAN) and the Vendor's User ID (UID). In addition, you will be required to enter the date you first entered into a provider agreement with this vendor and the name and email address of your authorized representative.
4. Log in to your MAC's HETS EDI enrollment portal.
The MACs which currently have an HETS EDI enrollment process are CEDI (jurisdictions JA - JD), National Government Services (J6/JK), Noridian EDISS (JE/JF), Novitas (JH/JL), First Coast Service Options (JN), Palmetto GBA (JJ/JM), CGS (J15) and WPS (J5/J8).
5. Complete and submit the attestation for each NPI.
Accept the HETS rules of behavior, download your Confirmation.
6. Verify completion.
Your vendor can verify that your NPI has been added to their Vendor UID by checking the HETS Desktop (HDT). Records update immediately.
Failure to enroll will allow for manual lookup of eligibility via the provider's secure online portal; however, it is a manual process that replaces what would be otherwise automated eligibility processes.
Therefore, teams responsible for management of their organization's medical account receivables services (billing) and are also responsible for front-end patient intake should consider this a critical component of their compliance workflow, rather than an IT side project.
Frequently Asked Questions About HETS EDI Attestation
All of your eligibility request submissions (for all of those NPIs) will have been denied due to an AAA error code of "41". Attestation does NOT provide a "grace" period. If you fail to attest before the deadline, you WILL lose eligibility check capability for the duration of this delay. During this delay in automated eligibility checking you MUST perform eligibility checks through your MAC's portal.
YES. Bulk attestation does NOT exist. Billing NPIs are required to link individually to each vendor or clearinghouse that submits eligibility inquiries on their behalf.
No. A clearinghouse is unable to attest on a provider's behalf. All providers will need to login, read the HETS rules of behavior, then individually enter their attestation.
No. Non-Medicare eligibility checks (including but not limited to Commercial, Medicaid and other) may be processed as normal. No changes have been made that would negatively impact these types of eligibility transactions. Only Medicare Fee-for-Service (FFS) eligibility transactions through HETS are subject to this new requirement.
The May 11th HETS EDI attestation deadline is probably the most straight-forward of the compliance deadlines CMS has issued - as long as you take action immediately. Healthcare organizations that will be struggling to keep up are those who have treated this like a low-priority it ticket. Missing one simple form could eliminate Medicare eligibility verification for your entire patient population. The team at Human Medical Billing works with practices and health systems across the country to stay ahead of exactly these kind of front-end compliance changes. If your medical billing services partner hasn't flagged this deadline yet, it is time to get in touch about this issue.

Contact Human Medical Billing to schedule a compliance readiness review or learn more about our end-to-end billing and regulatory support services.

